글로벌 연구동향
의학물리학
- [Front. Phys.] Radiotherapy Risk Estimation Based on Expert Group Survey방사선치료의 위험도는 얼마나 될까?
연세의대 / 구지혜, 김동욱*
- 출처
- Front. Phys.
- 등재일
- 2019 August 21
- 저널이슈번호
- https://doi.org/10.3389/fphy.2019.00118
- 내용
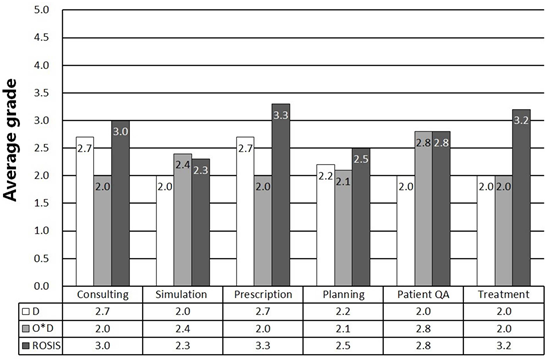
방사선치료과정을 총 6개의 단계로 나누고 총 144개 항목을 각 단계 별로 배치하여 국내 19명의 의학물리전문인이 FMEA에 따라 계산한 D( Detection)와 O(Occurrence) 및 O x D를 ROSIS 결과와 비교한 그래프입니다. D 값의 경우 Treatment 단계를 제외한 대부분의 단계에서 실제 ROSIS에서의 Event 분포와 비슷한 경향을 보여주고 있으며 본 연구가 의학물리전문인만으로 구성되어 진행되었다는 점과 유럽과 한국간의 치료 절차 및 시스템에서의 차이가 존재할 것이라는 점등을 고려하면 추후, 의사, 간호사, 방사선사 등을 포함하는 다양한 직종이 포함된 연구팀을 구성하고 국내 방사선치료사고 통계에 대한 연구를 수행한다면 그 결과가 매우 흥미로울 것으로 사료됩니다. 따라서, 현재 미국의 ROILS(Radiation Oncology Incident Learning System)와 유럽의 SAFRON(Safety in Radiation Oncology)과 같은 방사선사고 보고시스템의 국내도입 및 데이터베이스 구축이 매우 필요하다고 사료됩니다.
Abstract
Although current quality assurance systems such as Task Group 142 of the American Association of Physicists in Medicine and other methods used for radiotherapy have greatly contributed to decreasing radiotherapy incidents, there is still scope for improvement. In this study, we attempted to evaluate the reliability of the risk priority number, which was suggested by the AAPM Task Group 100, when it was calculated by an expert group in Korea. By doing this, we aimed at providing preliminary data for applying Failure Modes and Effect Analysis (FMEA), a systematic approach to identify potential failures in Korea. For this purpose, 1,163 incidents data in the Radiation Oncology Safety Information System (ROSIS) database were used. The incident data were categorized into 144 items to create a questionnaire. The expert group consisted of 19 physicists who evaluated the occurrence (O), severity (S), and detectability (D) of each item on a scale from 1 to 10 according to the AAPM Task Group 100. Among these three factors, the values of “O × D” were compared with ROSIS data. When comparing the O × D value between the items ranked in the top 10 of the survey and ROSIS data, no items were duplicated, and “simulation” and “treatment” were most frequent among, in total, eight processes. The average difference of O × D between the survey and ROSIS data was 0.8 ± 1.5, and this difference barely followed a Gaussian distribution. The results of this work indicates that FMEA is a good predictor, but that there were still deviations between actual risk and expectations in some cases, because actual incidents are multifactorial rather than simply proportional to D and O. Further research on radiotherapy risk estimation is needed.
Author information
Jihye Koo1, Dong Oh Shin2, Young Kyung Lim3, Soah Park4, Jeong Eun Rah5, Ui Jung Hwang6 and Dong Wook Kim7*
1Department of Physics, University of South Florida, Tampa, FL, United States
2Department of Radiation Oncology, Kyung Hee University Medical Center, Seoul, South Korea
3Proton Therapy Center, National Cancer Center Korea, Goyang, South Korea
4Department of Radiation Oncology, Hallym University College of Medicine, Seoul, South Korea
5Department of Radiation Oncology, Myongji Hospital, Goyang, South Korea
6Department of Radiation Oncology, Chungnam National University Hospital, Daejeon, South Korea
7Department of Radiation Oncology, Yonsei Cancer Center, Yonsei University College of Medicine, Seoul, South Korea
- 연구소개
- 방사선치료는 고령 인구와 암 환자 발병율의 증가, 방사선치료기기의 발전과 진화로 인하여 외과적 수술이나 항암치료와 더불어 중추적인 역할하고 있다. 방사선치료관련 학회나 국제기구에서 권고되고 있는 품질관리보고서(AAPM TG 142 등) 및 외부 감사는 방사선치료의 질적 향상 및 안전문화 정착에 크게 기여하였다. 이 논문은 ROSIS(Radiation Oncology Safety Information System)의 사건/사고 데이터(1,163건)를 이용하여 AAPM TG 100에 따라 국내 전문가 그룹(19명)의 설문 조사를 통해 방사선치료 전 과정에 대하여 고장/사건/사고 유형을 파악하여 영향을 분석하는 FMEA(Failure Modes and Effective Analysis)를 실시한 연구이다. 본 연구의 결과는 FMEA가 좋은 예측인자이기는 하지만, 실제 사건/사고는 단순히 각 분류 항목의 발생율(O)과 탐지 가능성(D)에 비례하기보다는 방사선치료는 복잡하고 다단계 프로세서에 의해 이루어지기 때문에 실제 위험도와 기대치 간에 여전히 편차가 있음을 확인한 논문이라고 생각된다. 그러므로 방사선치료의 품질관리 경향이 기계적인 품질관리에서 단계별 절차나 프로세스별 품질관리 또는 환자별 품질관리, 즉 리스크 관리로 패러다임이 전환되고 있는 상황에서 가까운 시일 내에 국내에서도 방사선치료에 있어 환자의 의료피폭 최적화 및 사건 사고를 예방하기 위해 암환자에 대한 국가적인 리스크 관리가 필요하다는 점을 제시하는 논문이라고 사료된다.
- 덧글달기
- 이전글 [Front Aging Neurosci.] Topographical Heterogeneity of Alzheimer's Disease Based on MR Imaging, Tau PET, and Amyloid PET.
- 다음글 [J Nucl Med.] Generation of PET Attenuation Map for Whole-Body Time-of-Flight 18F-FDG PET/MRI Using a Deep Neural Network Trained with Simultaneously Reconstructed Activity and Attenuation Maps.








편집위원
방사선치료는 다양한 전문 직종에 의해 환자에 대한 치료 처방과 영상 획득, 방사선치료계획 최적화, 치료 전 환자맞춤형 품질관리, 환자에게 방사선치료 행위를 수행하는 과정까지 복잡하고 다단계 프로세스로 수행되고 있다. 방사선치료 효과를 향상시키기 위해 고정밀 방사선치료기법이 임상에 널리 적용되고 있어 방사선치료기기에 대한 기계적/기하학적인 품질관리뿐만 아니라 사람 실수를 줄이기 위한 관심과 노력이 필요하다고 생각된다. 이 논문은 ROSIS 데이터를 토대로 AAPM TG 100에 따라 국내 전문가 그룹(의학물리전문인)의 설문 조사를 통해 FMEA를 실시한 연구 결과를 제시함으로써 흥미로웠다. 향후 국내에서도 방사선치료에 있어서 사건/사고를 미연에 방지하고 방사선치료의 질적 향상을 위해서는 학회 차원에 의한 방사선치료 프로세스별 리스크 관리가 필요하다고 사료된다.
2019-09-27 15:13:48
coque iphone pas che
How is Very last. fm not necessarily with this record... also, look at tuberadio. net daaah, considering that the name affirms: options to help the planet pandora and also LASTFM idiot!
[url=https://www.anten.fr/]coque iphone pas cher 6[/url]
2019-10-28 19:44:37
coque samsung a5 201
Justin, fantastic post. I had been utilizing Glass windows Storage Server 08 using ESXi 4. - Still immediately after upgrading for you to ESXi five. 0 We are acquiring difficulties. Such as the posting below:
<a href=https://www.anten.fr/collections/coque-samsung-a5 >coque samsung a5 2015</a>
2019-10-29 17:21:12